Mindfulness Improves Cognitive Function in Older Adults by Altering Brain Gene Expression
By John M. de Castro, Ph.D.
“mindfulness may target inflammation, stress-related pathways, and neuroplasticity, thus reducing the risk of developing cerebrovascular disease and age-related neurodegeneration that could lead to the development of dementia.” – Ted Kheng Siang Ng
The aging process involves a systematic progressive decline in every system in the body, the brain included. The elderly frequently have problems with attention, thinking, and memory abilities, known as mild cognitive impairment. An encouraging new development is that mindfulness practices such as meditation training and mindful movement practices can significantly reduce these declines in cognitive ability. In addition, it has been found that
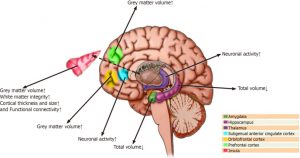
mindfulness practices reduce the deterioration of the brain that occurs with aging restraining the loss of neural tissue. Indeed, the brains of practitioners of meditation have been found to degenerate less with aging than non-practitioners. The mechanisms by which mindfulness affects the brain and reduces cognitive decline need to be investigated.
In today’s Research News article “Mindfulness intervention improves cognitive function in older adults by enhancing the level of miRNA-29c in neuron-derived extracellular vesicles.” (See summary below or view the full text of the study at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8575875/ ) Hashizume and colleagues recruited healthy elderly adults aged 65 and over and administered either 4 weeks , 3 times per week for 60 minutes of Mindfulness-Based Stress Reduction (MBSR) or a no-treatment wait-list condition. They were measured before and after treatment for cognitive function including delayed recall, visuospatial/executive function, attention, abstraction, language, naming, and orientation tasks. They also had blood drawn and assayed for extracellular vesicles and mRNA in the vesicles.
They found that in comparison to baseline and the wait list control, after Mindfulness-Based Stress Reduction (MBSR) there were significant improvement in cognitive function including delayed recall, visuospatial/executive function, attention, naming, and orientation tasks. The blood assays revealed that in comparison to baseline and the wait list control, after MBSR there were significant reductions in miR-29c in the extracellular vesicles and decreased expression of the genes DNMT3A, DNMT3B, and BACE1 in in the extracellular vesicles. In another study with mice they found that injection into the brain ventricles of miR-29c prevented cognitive decline in the animals.
The results suggest that mindfulness training improves cognitive function in the elderly. These improvements in cognition have been previously observed by other researchers. The new findings in the present research are the changes in the extracellular vesicles found in the plasma. The expression of the mRNA miR-29c controls the gene expressions of DNMT3A, DNMT3B, and BACE1. These genes are associated with the loss of neurons in the brain. With aging there is a degeneration of the brain including losses of neurons. Reductions in the expression of the genes that tend to produce neuronal loss after Mindfulness-Based Stress Reduction (MBSR) suggests that the training protects the brain from the loss of neurons. This may represent the mechanism by which mindfulness training protects the brain in aging individual which results in improved cognitive function. It may be how mindfulness training stops cognitive decline in the elderly.
So, mindfulness improves cognitive function in older adults by altering brain gene expression.
“an 8-week mindfulness-based training program improved cognition . . . in cognitively normal older adults, and that these improvements were associated with increased intrinsic connectivity within the default mode network.” – Gunes Sevinc
CMCS – Center for Mindfulness and Contemplative Studies
This and other Contemplative Studies posts are available on Twitter @MindfulResearch
Study Summary
Hashizume, S., Nakano, M., Kubota, K., Sato, S., Himuro, N., Kobayashi, E., Takaoka, A., & Fujimiya, M. (2021). Mindfulness intervention improves cognitive function in older adults by enhancing the level of miRNA-29c in neuron-derived extracellular vesicles. Scientific reports, 11(1), 21848. https://doi.org/10.1038/s41598-021-01318-y
Abstract
Although mindfulness-based stress reduction (MBSR) improves cognitive function, the mechanism is not clear. In this study, people aged 65 years and older were recruited from elderly communities in Chitose City, Japan, and assigned to a non-MBSR group or a MBSR group. Before and after the intervention, the Japanese version of the Montreal Cognitive Assessment (MoCA-J) was administered, and blood samples were collected. Then, neuron-derived extracellular vesicles (NDEVs) were isolated from blood samples, and microRNAs, as well as the target mRNAs, were evaluated in NDEVs. A linear mixed model analysis showed significant effects of the MBSR x time interaction on the MoCA-J scores, the expression of miRNA(miR)-29c, DNA methyltransferase 3 alpha (DNMT3A), and DNMT3B in NDEVs. These results indicate that MBSR can improve cognitive function by increasing the expression of miR-29c and decreasing the expression of DNMT3A, as well as DNMT3B, in neurons. It was also found that intracerebroventricular injection of miR-29c mimic into 5xFAD mice prevented cognitive decline, as well as neuronal loss in the subiculum area, by down-regulating Dnmt3a and Dnmt3b in the hippocampus. The present study suggests that MBSR can prevent neuronal loss and cognitive impairment by increasing the neuronal expression of miR-29c.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8575875/