Meditation Effects on Mindfulness and Emotion Regulation are Associated with Changes in Brain Activity
By John M. de Castro, Ph.D.
“the meditation intervention had large varying effects on EEG spectra, . . Findings suggest that brief guided meditation intervention may offer positive and immediate health benefits to help combat stress.” – Peta Stapleton
Meditation training has been shown to improve health and well-being. It has also been found to be effective for a large array of medical and psychiatric conditions, either stand-alone or in combination with more traditional therapies. There are several ways that meditation practices produce these benefits, including changes to the brain and physiology. One way to observe the effects of meditation on neural activity is to measure changes in the electroencephalogram (EEG), the rhythmic electrical activity that can be recorded from the scalp.
The recorded activity can be separated into frequency bands. Delta activity consists of oscillations in the 0.5-3 cycles per second band. Theta activity in the EEG consists of oscillations in the 4-8 cycles per second band. Alpha activity consists of oscillations in the 8-12 cycles per second band. Beta activity consists of oscillations in the 15-25 cycles per second band while Gamma activity occurs in the 35-45 cycles per second band. There needs to be further research on how changes in brain activity progress a meditation practice develops.
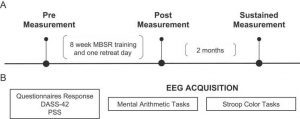
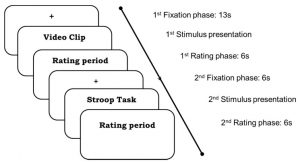
In today’s Research News article “Mindfulness Training Associated With Resting-State Electroencephalograms Dynamics in Novice Practitioners via Mindful Breathing and Body-Scan.” (See summary below or view the full text of the study at: https://www.frontiersin.org/articles/10.3389/fpsyg.2021.748584/full?utm_source=F-AAE&utm_medium=EMLF&utm_campaign=MRK_1765474_a0P58000000G0YfEAK_Psycho_20211102_arts_A ) Ng and colleagues recruited meditation naive healthy adults and randomly assigned them to either a wait-list control condition or to receive 8 weekly 2,5 hour sessions of Mindfulness-Based Stress Reduction (MBSR). The intervention consisted of meditation, body scan, and yoga along with group discussion and home practice. Before and after the 8-week program they were measured for mindfulness and emotion regulation and underwent simultaneous brain scanning with functional magnetic resonance imaging (fMRI) and brain electrical activity measurement with electroencephalogram (EEG). The scanning occurred with 5-minute epochs of rest, mindful breathing, body scan, and rest during which they were asked to press a button whenever their mind wandered.
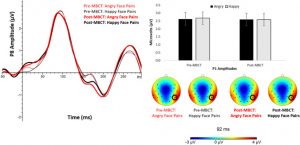
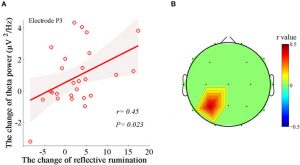
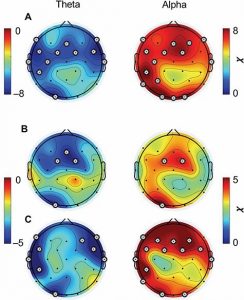
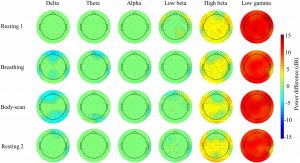
They found that in comparison to baseline and the wait-list control group the group that received Mindfulness-Based Stress Reduction (MBSR) had significantly greater levels of mindfulness and emotion regulation. In the electroencephalogram (EEG) after MBSR training there were significant increases in power in the beta and gamma bands and decreases in the delta band in the frontal and parietal cortex regardless of condition. They also found that in comparison to the resting condition during body scan the MBSR group had significantly lower power in the delta, beta, and gamma bands. Changes in the EEG powers were significantly related to changes in mindfulness and emotion regulation.
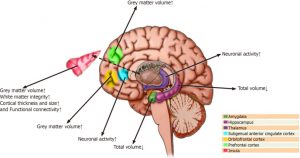
The present results are similar to previous findings that mindfulness training produces significant improvements in mindfulness and emotion regulation. But the present findings are unique in showing that these changes are associated with changes in the electroencephalogram (EEG) produced by mindfulness training. Since the participants were meditation naïve at the beginning, these findings document how mindfulness training may produce its benefits. They suggest that mindfulness training alters brain processing increasing spectral power in the brain and this produces changes in psychological processes.
Hence, meditation effects on mindfulness and emotion regulation are associated with changes in brain activity.
“Many studies on mindfulness meditation have linked lower frequency alpha waves, as well as theta waves, to meditation.” – Wikipedia
CMCS – Center for Mindfulness and Contemplative Studies
This and other Contemplative Studies posts are available at the Contemplative Studies Blog http://contemplative-studies.org/wp/
They are also available on Google+ https://plus.google.com/106784388191201299496/posts and on Twitter @MindfulResearch
Study Summary
Ng H-YH, Wu CW, Huang F-Y, Cheng Y-T, Guu S-F, Huang C-M, Hsu C-F, Chao Y-P, Jung T-P and Chuang C-H (2021) Mindfulness Training Associated With Resting-State Electroencephalograms Dynamics in Novice Practitioners via Mindful Breathing and Body-Scan. Front. Psychol. 12:748584. doi: 10.3389/fpsyg.2021.748584
Objectives: Mindfulness-based stress reduction has been proven to improve mental health and quality of life. This study examined how mindfulness training and various types of mindfulness practices altered brain activity.
Methods: Specifically, the spectral powers of scalp electroencephalography of the mindfulness-based stress reduction (MBSR) group (n=17) who underwent an 8-week MBSR training—including mindful breathing and body-scan—were evaluated and compared with those of the waitlist controls (n=14).
Results: Empirical results indicated that the post-intervention effect of MBSR significantly elevated the resting-state beta powers and reduced resting-state delta powers in both practices; such changes were not observed in the waitlist control. Compared with mindful breathing, body-scanning resulted in an overall decline in electroencephalograms (EEG) spectral powers at both delta and low-gamma bands among trained participants.
Conclusion: Together with our preliminary data of expert mediators, the aforementioned spectral changes were salient after intervention, but mitigated along with expertise. Additionally, after receiving training, the MBSR group’s mindfulness and emotion regulation levels improved significantly, which were correlated with the EEG spectral changes in the theta, alpha, and low-beta bands. The results supported that MBSR might function as a unique internal processing tool that involves increased vigilant capability and induces alterations similar to other cognitive training.
https://www.frontiersin.org/articles/10.3389/fpsyg.2021.748584/full?utm_source=F-AAE&utm_medium=EMLF&utm_campaign=MRK_1765474_a0P58000000G0YfEAK_Psycho_20211102_arts_A
By John M. de Castro, Ph.D.
“the meditation intervention had large varying effects on EEG spectra, . . Findings suggest that brief guided meditation intervention may offer positive and immediate health benefits to help combat stress.” – Peta Stapleton
Meditation training has been shown to improve health and well-being. It has also been found to be effective for a large array of medical and psychiatric conditions, either stand-alone or in combination with more traditional therapies. There are several ways that meditation practices produce these benefits, including changes to the brain and physiology. One way to observe the effects of meditation on neural activity is to measure changes in the electroencephalogram (EEG), the rhythmic electrical activity that can be recorded from the scalp.
The recorded activity can be separated into frequency bands. Delta activity consists of oscillations in the 0.5-3 cycles per second band. Theta activity in the EEG consists of oscillations in the 4-8 cycles per second band. Alpha activity consists of oscillations in the 8-12 cycles per second band. Beta activity consists of oscillations in the 15-25 cycles per second band while Gamma activity occurs in the 35-45 cycles per second band. There needs to be further research on how changes in brain activity progress a meditation practice develops.
In today’s Research News article “Mindfulness Training Associated With Resting-State Electroencephalograms Dynamics in Novice Practitioners via Mindful Breathing and Body-Scan.” (See summary below or view the full text of the study at: https://www.frontiersin.org/articles/10.3389/fpsyg.2021.748584/full?utm_source=F-AAE&utm_medium=EMLF&utm_campaign=MRK_1765474_a0P58000000G0YfEAK_Psycho_20211102_arts_A ) Ng and colleagues recruited meditation naive healthy adults and randomly assigned them to either a wait-list control condition or to receive 8 weekly 2,5 hour sessions of Mindfulness-Based Stress Reduction (MBSR). The intervention consisted of meditation, body scan, and yoga along with group discussion and home practice. Before and after the 8-week program they were measured for mindfulness and emotion regulation and underwent simultaneous brain scanning with functional magnetic resonance imaging (fMRI) and brain electrical activity measurement with electroencephalogram (EEG). The scanning occurred with 5-minute epochs of rest, mindful breathing, body scan, and rest during which they were asked to press a button whenever their mind wandered.
They found that in comparison to baseline and the wait-list control group the group that received Mindfulness-Based Stress Reduction (MBSR) had significantly greater levels of mindfulness and emotion regulation. In the electroencephalogram (EEG) after MBSR training there were significant increases in power in the beta and gamma bands and decreases in the delta band in the frontal and parietal cortex regardless of condition. They also found that in comparison to the resting condition during body scan the MBSR group had significantly lower power in the delta, beta, and gamma bands. Changes in the EEG powers were significantly related to changes in mindfulness and emotion regulation.
The present results are similar to previous findings that mindfulness training produces significant improvements in mindfulness and emotion regulation. But the present findings are unique in showing that these changes are associated with changes in the electroencephalogram (EEG) produced by mindfulness training. Since the participants were meditation naïve at the beginning, these findings document how mindfulness training may produce its benefits. They suggest that mindfulness training alters brain processing increasing spectral power in the brain and this produces changes in psychological processes.
Hence, meditation effects on mindfulness and emotion regulation are associated with changes in brain activity.
“Many studies on mindfulness meditation have linked lower frequency alpha waves, as well as theta waves, to meditation.” – Wikipedia
CMCS – Center for Mindfulness and Contemplative Studies
This and other Contemplative Studies posts are also available on Google+ https://plus.google.com/106784388191201299496/posts and on Twitter @MindfulResearch
Study Summary
Ng H-YH, Wu CW, Huang F-Y, Cheng Y-T, Guu S-F, Huang C-M, Hsu C-F, Chao Y-P, Jung T-P and Chuang C-H (2021) Mindfulness Training Associated With Resting-State Electroencephalograms Dynamics in Novice Practitioners via Mindful Breathing and Body-Scan. Front. Psychol. 12:748584. doi: 10.3389/fpsyg.2021.748584
Objectives: Mindfulness-based stress reduction has been proven to improve mental health and quality of life. This study examined how mindfulness training and various types of mindfulness practices altered brain activity.
Methods: Specifically, the spectral powers of scalp electroencephalography of the mindfulness-based stress reduction (MBSR) group (n=17) who underwent an 8-week MBSR training—including mindful breathing and body-scan—were evaluated and compared with those of the waitlist controls (n=14).
Results: Empirical results indicated that the post-intervention effect of MBSR significantly elevated the resting-state beta powers and reduced resting-state delta powers in both practices; such changes were not observed in the waitlist control. Compared with mindful breathing, body-scanning resulted in an overall decline in electroencephalograms (EEG) spectral powers at both delta and low-gamma bands among trained participants.
Conclusion: Together with our preliminary data of expert mediators, the aforementioned spectral changes were salient after intervention, but mitigated along with expertise. Additionally, after receiving training, the MBSR group’s mindfulness and emotion regulation levels improved significantly, which were correlated with the EEG spectral changes in the theta, alpha, and low-beta bands. The results supported that MBSR might function as a unique internal processing tool that involves increased vigilant capability and induces alterations similar to other cognitive training.
https://www.frontiersin.org/articles/10.3389/fpsyg.2021.748584/full?utm_source=F-AAE&utm_medium=EMLF&utm_campaign=MRK_1765474_a0P58000000G0YfEAK_Psycho_20211102_arts_A