By John M. de Castro, Ph.D.
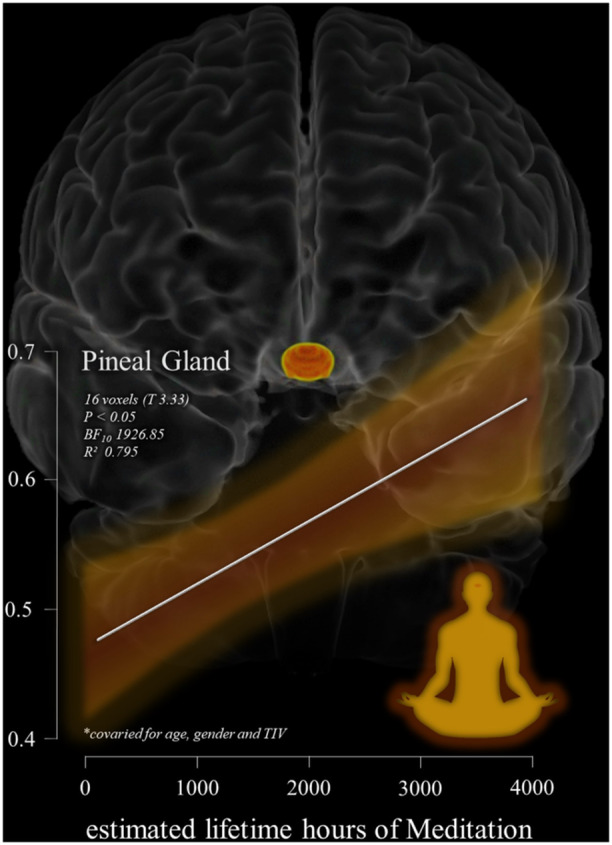
In today’s Research News article “A comparative study of the impact of meditation and Buddhist five precepts on stress and depression between older adults and younger adults.” (See summary below or view the full text of the study at: https://pmc.ncbi.nlm.nih.gov/articles/PMC12053757/) Wongpakaran and colleagues investigated the relationships between meditation and the practice of the five precepts on stress and depression in older (average 68 years) and younger (average 29 years) adults. The five precepts involve refraining from killing or harming living beings, stealing or taking others’ property without permission, engaging in sexual misconduct, speaking falsely, and consuming alcohol or intoxicants. They report that meditation and the practice of the five precepts enhances the reductions in stress and depression in older but not younger adults.
Meditation and practice of the five precepts reduces stress and depression in older adults.
CMCS – Center for Mindfulness and Contemplative Studies
This and other Contemplative Studies posts are also available on the Contemplative Studies Blog http://contemplative-studies.org
Study Summary
Wongpakaran N, Klaychaiya S, Panuspanudechdamrong C, et al. A comparative study of the impact of meditation and Buddhist five precepts on stress and depression between older adults and younger adults. Sci Rep. 2025;15(1):15739. Published 2025 May 6. doi:10.1038/s41598-025-99430-w
Abstract
Older adults frequently face a myriad of physical and mental health challenges, which can contribute to feelings of stress and subsequent depression. Nevertheless, with age often comes a wealth of life experience and resilience. Perceived stress commonly predicts depression across all age groups, while meditation has been associated with lower levels of depression. Additionally, adherence to the Five Precepts is a prevalent practice among Thai individuals, particularly among older adults. However, it remains unclear how the combination of meditation and the Buddhist Five Precepts influences depression levels. This study aims to explore the predictive roles of meditation, the practice of the Five Precepts, and perceived stress on depression among older adults, with comparisons drawn to younger adults. A sample of 1472 individuals (232 were older adults and 1240 were adults) participated in the study. All completed the questionnaires for depression, perceived stress, meditation, and five precepts using the core symptom index, perceived stress scale, and inner strength-based inventory. Moderation model and mediation model analyses were employed to analyze the relationship between the perceived stress scores and the symptoms of depression for both older and younger samples. In the older adults group, 59.9% were female, with a mean age of 67.96 years (SD 6.8). In the adult group, 71.3% were male, with a mean age of 29.04 years (SD 10.5). The findings revealed that among the older adults’ group, precepts, meditation, and their interaction significantly predicted a lower level of depressive symptoms (estimated coefficient = − 0.1082, 95% CI = − 0.1865, − 0.03). However, this association was not observed in the younger adults’ group (estimated coefficient = -0.0199, 95% CI = − 0.0465, 0.0066). The variance explained in depressive symptoms changed from 24.9% in the linear model of perceived stress to 31.8% in the moderated moderation model, representing a 27.7% increase. Conversely, meditation and the five precepts mediated the relationship between stress and depressive symptoms in younger people but not in older adults. The indirect effect of perceived stress was significant only through the five precepts (estimated coefficient = − 0.3173, 95% CI = − 0.4787, − 0.1558; p = .0001). The variance explained in depressive symptoms changed from 42.2% in the linear model of perceived stress to 43.2% in the mediation model, representing a 2.5% increase. This study emphasizes that older adults may experience enhanced benefits from meditation and adherence to the Five Precepts compared to younger adults. Additionally, the effectiveness of meditation appears to be influenced by the extent of precept practice. Older individuals who actively engage in both high levels of precept adherence and meditation demonstrate a more significant buffering effect on the relationship between stress and depression. These findings suggest that lifestyle factors, such as religious practices like meditation and adherence to precepts, may have a differential impact on older adults compared to younger counterparts. The implications for older individuals are promising and warrant encouragement, while further research is needed to explore relevant factors contributing to reduced depression among younger populations.