Improve Balance in Parkinson’s Disease with Tai Chi and Yoga
By John M. de Castro, Ph.D.
“In addition to easing balance problems, and possibly other symptoms, tai chi can help ease stress and anxiety and strengthen all parts of the body, with few if any harmful side effects. . . with Parkinson’s disease.” – Peter Wayne
Parkinson’s Disease (PD) is an incurable progressive degenerative disease of the central nervous system. The condition is caused by the death of nerve cells in the brain that produce the neurotransmitter dopamine. There are around seven million people worldwide and one million people in the U.S. living with PD and about 60,000 people are diagnosed with PD every year. PD is associated with aging as the vast majority of patients are diagnosed after age 50. In fact, it has been speculated that everyone would eventually develop PD if they lived long enough.
Its physical symptoms include resting tremor, slow movements, muscle rigidity, problems with posture and balance, loss of automatic movements, and slurring of speech. PD itself is not fatal but is often associated with related complications which can reduce life expectancy, such as falls, choking, and cardiovascular problems. PD also has psychological effects, especially cognitive decline, anxiety, and depression. Balance is a particular problem as it effects mobility and increases the likelihood of falls, restricting activity and reducing quality of life.
There are no cures for Parkinson’s Disease (PD) or even treatments to slow its progression. There are only treatments that can produce symptomatic relief. So, there is a need to discover new and different treatments. Mindfulness training has been found to improve the psychological symptoms and the quality of life with PD patients. In addition, Tai Chi and yoga practices have been shown to improve the symptoms of Parkinson’s Disease. Hence, mind-body practices may be excellent treatments for the symptoms of PD. It is important to discover which of various exercises works best to improve balance and mobility in patients with PD.
In today’s Research News article “Effect of home-based Tai Chi, Yoga or conventional balance exercise on functional balance and mobility among persons with idiopathic Parkinson’s disease: An experimental study.” (See summary below or view the full text of the study at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7136531/), Khuzema and colleagues recruited adult patients with Parkinson’s Disease and randomly assigned them to receive 5 days per week for 8 weeks for 30-40 minutes of either home based Tai Chi exercise, yoga exercise, or balance exercise training. They were measured before and after training for balance and mobility with a timed up and go test and a 10-minute walking test.
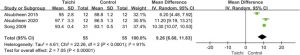
They found that all three exercise programs produced significant improvements in all measures. Balance increased significantly by 26.414%, 8.193% and 14.339%, Timed up and go time decreased by 22.695%, 7.187% and 8.902%, and 10-m Walk Time decreased by 24.469%, 5.914% and 8.986% in Tai Chi, yoga and balance exercise groups, respectively. Although, on average, Tai Chi exercise produced superior results on all measures, the study was too small (9 patients per group) to determine significant group differences. These results, however, support conducting a large randomized controlled trial in the future.
Tai Chi is an ancient mindfulness practice that involves slow prescribed movements. It is gentle and completely safe, can be used with the elderly and sickly, are inexpensive to administer, can be performed in groups or alone, at home or in a facility or even public park, and can be quickly learned. In addition, it can be practiced in social groups without professional supervision. This can make it fun, improving the likelihood of long-term engagement in the practice. Hence Tai Chi training should be recommended to improve balance and mobility in patients with Parkinson’s Disease.
So, improve balance in Parkinson’s Disease with Tai Chi and Yoga.
“Benefits of Tai Chi and Yoga for those with Parkinson’s Disease:
- Promotes conscious awareness of movement and actions.
- Increases awareness of proper body alignment/posture
- Improves balance with reduced fall risk
- Enhances flexibility
- Affords a greater sense of well-being
- Offers relaxation which can help to lessen Parkinson’s symptoms (tremor, rigidity) or manage medication side effects such as dyskinesia
- Improves breath support and control
- Helps to build healthy bones through weight-bearing activities
- Increases strength, especially in core muscles” – National Parkinson’s Foundation
CMCS – Center for Mindfulness and Contemplative Studies
This and other Contemplative Studies posts are also available on Google+ https://plus.google.com/106784388191201299496/posts and on Twitter @MindfulResearch
Study Summary
Khuzema, A., Brammatha, A., & Arul Selvan, V. (2020). Effect of home-based Tai Chi, Yoga or conventional balance exercise on functional balance and mobility among persons with idiopathic Parkinson’s disease: An experimental study. Hong Kong physiotherapy journal : official publication of the Hong Kong Physiotherapy Association Limited = Wu li chih liao, 40(1), 39–49. https://doi.org/10.1142/S1013702520500055
Abstract
Background:
Individuals with Parkinson’s disease (PD) invariably experience functional decline in a number of motor and non-motor domains affecting posture, balance and gait. Numerous clinical studies have examined effects of various types of exercise on motor and non-motor problems. But still much gap remains in our understanding of various therapies and their effect on delaying or slowing the dopamine neuron degeneration. Recently, Tai Chi and Yoga both have gained popularity as complementary therapies, since both have components for mind and body control.
Objective:
The aim of this study was to determine whether eight weeks of home-based Tai Chi or Yoga was more effective than regular balance exercises on functional balance and mobility.
Methods:
Twenty-seven individuals with Idiopathic PD (Modified Hoehn and Yahr stages 2.5–3) were randomly assigned to either Tai Chi, Yoga or Conventional exercise group. All the participants were evaluated for Functional Balance and Mobility using Berg Balance Scale, Timed 10 m Walk test and Timed Up and Go test before and after eight weeks of training.
Results:
The results were analyzed using two-way mixed ANOVA which showed that there was a significant main effect for time as F (1, 24) =74.18, p=0.000, ηp2=0.76 for overall balance in Berg Balance Scale. There was also significant main effect of time on mobility overall as F(1, 24) =77.78, p=0.000, ηp2=0.76 in Timed up and Go test and F(1, 24) =48.24, p=0.000, ηp2=0.67 for 10 m Walk test. There was a significant interaction effect for time×group with F(2, 24) =8.67, p=0.001, ηp2=0.420 for balance. With respect to mobility, the values F(2, 24) =5.92, p=0.008, ηp2=0.330 in Timed Up and Go test and F(2, 24) =10.40, p=0.001, ηp2=0.464 in 10 m Walk test showed a significant interaction. But there was no significant main effect between the groups for both balance and mobility.
Conclusion:
The findings of this study suggest that Tai Chi as well as Yoga are well adhered and are attractive options for a home-based setting. As any form of physical activity is considered beneficial for individuals with PD either Tai Chi, Yoga or conventional balance exercises could be used as therapeutic intervention to optimize balance and mobility. Further studies are necessary to understand the mind–body benefits of Tai Chi and Yoga either as multicomponent physical activities or as individual therapies in various stages of PD.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7136531/