Improve Glycemic Control in Patients with Type 2 Diabetes with Tai Chi
By John M. de Castro, Ph.D.
“Tai chi does not mean oriental wisdom or something exotic. It is the wisdom of your own senses, your own mind and body together as one process.” – Chungliang Al Huang
Diabetes is a major health issue. It is estimated that 30 million people in the United States have diabetes and the numbers are growing. Type 2 Diabetes results from a resistance of tissues, especially fat tissues, to the ability of insulin to promote the uptake of glucose from the blood. As a result, blood sugar levels rise producing hyperglycemia. Diabetes is the 7th leading cause of death in the United States. In addition, diabetes is heavily associated with other diseases such as cardiovascular disease, heart attacks, stroke, blindness, kidney disease, and circulatory problems leading to amputations. As a result, diabetes doubles the risk of death of any cause compared to individuals of the same age without diabetes.
Type 2 diabetes is largely preventable. One of the reasons for the increasing incidence of Type 2 Diabetes is its association with overweight and obesity which is becoming epidemic in the industrialized world. A leading cause of this is a sedentary lifestyle. Current treatments for Type 2 Diabetes focus on diet, exercise, and weight control. Recently, mindfulness practices have been shown to be helpful in managing diabetes. Tai Chi is mindfulness practice and a gentle exercise that has been found to improve the symptoms of Type 2 Diabetes. The research is accumulating. So, it is reasonable to examine what has been learned
In today’s Research News article “Effect of tai chi on glycaemic control, lipid metabolism and body composition in adults with type 2 diabetes: A meta-analysis and systematic review.” (See summary below or view the full text of the study at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8814847/ ) Guo and colleagues review, summarize, and perform a meta-analysis of the published research studies of the effectiveness of Tai Chi practice in the treatment of Type 2 Diabetes. They identified 23 published randomized clinical trials.
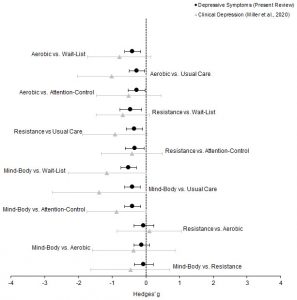
They report that the published research found that in comparison to usual clinical care, patients who were given Tai Chi practice had significantly lower levels of body mass index, systolic and diastolic blood pressure, insulin levels, fasting blood glucose, blood glucose levels after meals, HbA1c, total cholesterol, and low density lipoproteins (LDL), and higher levels of high density lipoproteins (HDL). Tai Chi produced similar results in comparison to aerobic exercise with body mass index, fasting blood glucose levels, total cholesterol, triglycerides, and low-density lipoproteins (LDL). Tai Chi produced superior results to aerobic exercise in reducing HbA1c and increasing high density lipoproteins (HDL).
Hence, the research published to date indicates that Tai Chi practice is superior to usual clinical care in improving obesity, glycemic control, and plasma fats and is superior to aerobic exercise in improving glycemic control and blood fats. This suggests that Tai Chi practice should be recommended for patients with Type 2 Diabetes.
“Tai Chi Chuan, the great ultimate, strengthens the weak, raises the sick, invigorates the debilitated, and encourages the timid.” – Cheng Man-ch’ing
CMCS – Center for Mindfulness and Contemplative Studies
This and other Contemplative Studies posts are also available on Twitter @MindfulResearch
Study Summary
Guo S, Xu Y, Qin J, Chen Y, You Y, Tao J, Liu Z, Huang J. Effect of tai chi on glycaemic control, lipid metabolism and body composition in adults with type 2 diabetes: A meta-analysis and systematic review. J Rehabil Med. 2021 Mar 22;53(3):jrm00165. doi: 10.2340/16501977-2799. PMID: 33594445; PMCID: PMC8814847.
Abstract
Objective
The aim of this systematic review was to evaluate the effects of tai chi on metabolic control and body composition indicators in patients with type 2 diabetes mellitus.
Design
Systematic review and meta-analysis of existing literature.
Methods
Electronic resource databases were searched to collect eligible studies. Two reviewers selected studies and independently evaluated methodological quality.
Results
Twenty-three studies were included in this meta-analysis. The pooled results showed that tai chi had significant effects in improving metabolic indices, such as fasting blood glucose (mean difference (MD) = –1.04; 95% confidence interval (95% CI) –1.42 to 0.66; p < 0.01) and total cholesterol (MD = –0.50; 95% CI –0.86 to –0.13; p < 0.01) compared with conventional clinical therapy. Most indices did not support the use of tai chi over aerobic exercise, except for glycated haemoglobin (HbA1c) (MD = –0.24; 95% CI –0.49 to 0.00; p < 0.01) and high-density lipoprotein (MD = 0.07; 95% CI 0.01 to 0.12; p < 0.01).
Conclusion
Tai chi had better effects on metabolic control and body composition indicators than clinical conventional therapy, but only on HbA1c and HDL were superior than that of aerobic exercise. The best time-window for tai chi intervention may differ with different metabolic indices.
LAY ABSTRACT
Exercise therapy is a possible alternative and effective strategy for blood glucose control in patients with type 2 diabetes, since drug therapy is associated with side-effects, long-term loss of efficacy, and poor adherence to lifelong treatment. A review of evidence was performed regarding the effects of tai chi on glycaemic control and other indicators in patients with type 2 diabetes mellitus. The results indicate that tai chi not only improves metabolic control, e.g. fasting blood glucose and total cholesterol, but also improves body composition indicators, e.g. body mass index. However, benefits of tai chi over aerobic exercise were seen in only a few outcome measures. The type and methodology of studies varied widely, with discrepancies in intensity, frequency, and duration of tai chi; therefore, further high-quality research is needed in order to draw specific and accurate conclusions.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8814847/