Mind-Body Skills Training Improves College Student Mental Health and Well-Being
By John M. de Castro, Ph.D.
“By focusing on and controlling our breath, we can change how we think and feel. We can use the breath as a means of changing our emotional state and managing stress.” —Tommy Rosen
There is an accumulating volume of research findings to demonstrate that Mind-body practices have highly beneficial effects on the health and well-being of humans. These include meditation, yoga, tai chi, qigong, biofeedback, progressive muscle relaxation, guided imagery, hypnosis, and deep breathing exercises. Because of their proven benefits the application of these practices to relieving human suffering has skyrocketed.
There is a lot of pressure on college students to excel. This stress might in fact be counterproductive as the increased pressure can actually lead to stress and anxiety which can impede the student’s physical and mental health, well-being, and school performance. Mindfulness training has been shown through extensive research to be effective in improving physical and psychological health. Indeed, these practices have been found to improve psychological health in college students. So, it would be expected that training in mind-body practices would improve the psychological health of college students.
In today’s Research News article “Impact of a University-Wide Interdisciplinary Mind-Body Skills Program on Student Mental and Emotional Well-Being.” (See summary below or view the full text of the study at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7686595/ ) Novak and colleagues recruited college students who were enrolled to take a mind-body skills program and an equivalent group of control college students. The program consisted of 9-weeks of once a week for 2 hours training and discussion of “mindfulness, guided imagery, autogenic training, biofeedback, and breathing techniques, as well as art, music, and movement practices” in groups of 10. The students were instructed to practice daily at home for 20 minutes. They were measured before and after training for perceived stress, positive and negative emotions, resilience, depression, anxiety, fatigue, sleep disturbance, mindfulness, interpersonal reactivity, and burnout. Subsets of each group were remeasured one year after the completion of the study. There were no significant differences in these measures between the groups at baseline.
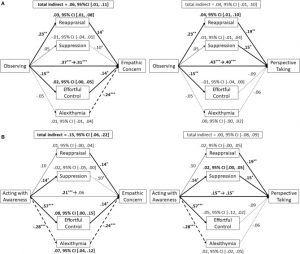
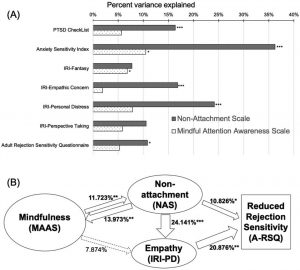
They found that in comparison to the baseline and the control group, the students who received mind-body skills training had significant decreases in perceived stress, negative affect, depression, anxiety, sleep disturbance, and burnout and significant increases in positive emotions, resilience, mindfulness, empathic concern, and perspective taking. In addition, the higher the levels of mindfulness the lower the levels of perceived stress, negative emotions and depersonalization and the higher the levels of positive emotions, resilience, and perspective taking. Unfortunately, these improvements, except for mindfulness, disappeared by the one year follow up.
The present study did not have an active control condition. So, it is possible that confounding factors such as participant expectancy, experimenter bias, attention effects etc. may have been responsible for the results. But in prior controlled research it has been demonstrated that mindfulness training produces decreases in perceived stress, negative emotions, depression, anxiety, sleep disturbance, and burnout and significant increases in positive emotions, resilience, and empathic concern. So, it is likely that the benefits observed in the present study were due to the mind-body skills training.
These results then suggest that mind-body skills training produces marked improvements in the psychological health and well-being of college students. But the improvements were not lasting. This may signal the need for better training protocols or periodic booster session to maintain the benefits. Given the great academic stress, pressure, and social stresses of college life, the students were much better off for taking the mind-body skills training program. It was not measured but these benefits would predict increased academic performance and improved well-being in these students.
So, mind-body skills training improves college student mental health and well-being.
“mind/body approaches to healing and wellness are gaining in popularity in the U.S. and research supports their efficacy in treating a number of psychological and physical health issues that are not easily treated by mainstream medicine.” – Doug Guiffrida
CMCS – Center for Mindfulness and Contemplative Studies
This and other Contemplative Studies posts are a also available on Google+ https://plus.google.com/106784388191201299496/posts and on Twitter @MindfulResearch
Study Summary
Novak, B. K., Gebhardt, A., Pallerla, H., McDonald, S. B., Haramati, A., & Cotton, S. (2020). Impact of a University-Wide Interdisciplinary Mind-Body Skills Program on Student Mental and Emotional Well-Being. Global Advances in Health and Medicine, 9, 2164956120973983. https://doi.org/10.1177/2164956120973983
Abstract
Background
Positive effects of mind-body skills programs on participant well-being have been reported in health professions students. The success seen with medical students at this university led to great interest in expanding the mind-body skills program so students in other disciplines could benefit from the program.
Objective
The purpose of this study was to assess the effects of a 9-week mind-body skills program on the mental and emotional well-being of multidisciplinary students compared to controls. We also sought to determine if the program’s effects were sustained at 1-year follow-up.
Methods
A cross-sectional pre-post survey was administered online via SurveyMonkey to participants of a 9-week mind-body skills program and a control group of students from 7 colleges at a public university from 2017–2019. Students were assessed on validated measures of stress, positive/negative affect, resilience, depression, anxiety, fatigue, sleep disturbance, mindfulness, empathy, and burnout. Scores were analyzed between-groups and within-groups using bivariate and multivariate analyses. A 1-year follow-up was completed on a subset of participants and controls.
Results
279 participants and 247 controls completed the pre-survey and post-survey (79% response rate; 71% female, 68% white, mean age = 25 years). Participants showed significant decreases in stress, negative affect, depression, anxiety, sleep disturbance, and burnout, while positive affect, resilience, mindfulness, and empathy increased significantly (P < .05). Only sleep disturbance showed a significant decrease in the control group. Follow-up in a subset of participants showed that only mindfulness remained elevated at 1-year (P < .05), whereas the significant changes in other well-being measures were not sustained.
Conclusion
Participation in a 9-week mind-body skills program led to significant improvement in indicators of well-being in multidisciplinary students. A pilot 1-year follow-up suggests that effects are only sustained for mindfulness, but not other parameters. Future programming should focus on implementing mind-body skills booster sessions to help sustain the well-being benefits.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7686595/