By John M. de Castro, Ph.D.
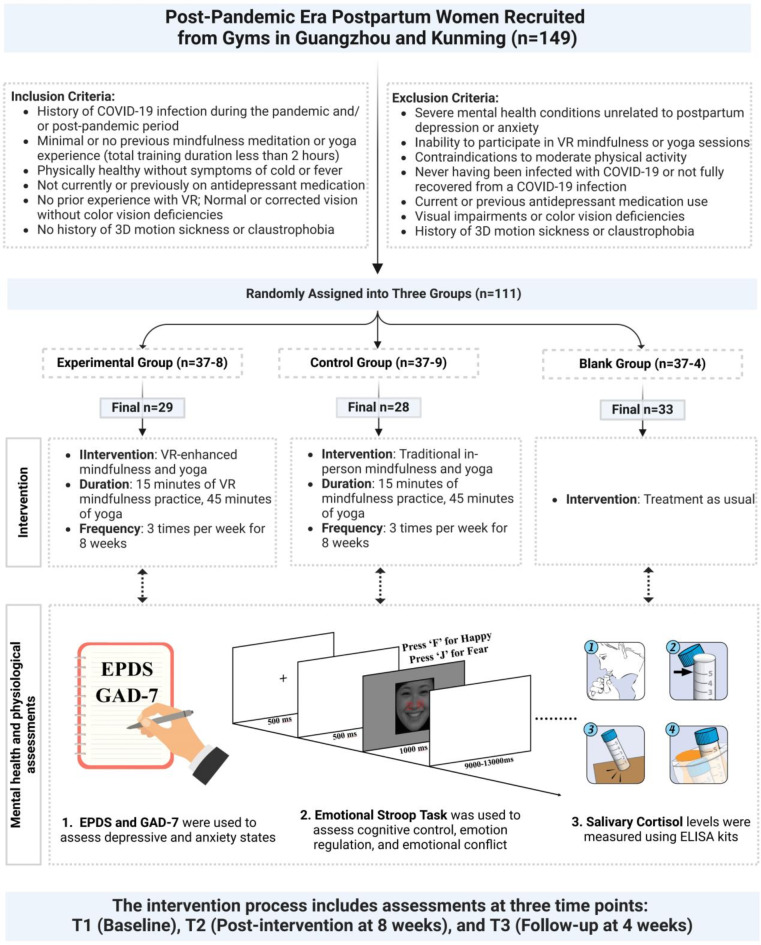
In today’s Research News article “Enhancing Quality of Life in Patients With Hypothyroidism Using a Scientific Yoga Module: Randomized Controlled Trial” (See summary below or view the full text of the study at: https://pmc.ncbi.nlm.nih.gov/articles/PMC12246764/) Nilkantham and colleagues performed a clinical trial of the effectiveness of 6 months of yoga practice presented over the internet in comparison to a wait-list control condition on the physical and psychological well-being of patients with hypothyroidism. They found that telehealth yoga resulted in significant improvements in mental health, energy, vitality, and role limitations.
Tele-Yoga is an effective treatment for the psychological symptoms of hypothyroidism.
CMCS – Center for Mindfulness and Contemplative Studies
This and other Contemplative Studies posts are also available on the Contemplative Studies Blog http://contemplative-studies.org
Study Summary
Nilkantham S, Singh A, Majumdar V, K N H, Atmakur S. Enhancing Quality of Life in Patients With Hypothyroidism Using a Scientific Yoga Module: Randomized Controlled Trial. J Med Internet Res. 2025 Jun 26;27:e54078. doi: 10.2196/54078. PMID: 40570327; PMCID: PMC12246764.
Abstract
Background
The impact of hypothyroidism on quality of life is extensively documented, highlighting its substantial physical, psychological, and social burden. Yoga has demonstrated promising therapeutic benefits in improving hypothyroidism outcomes. Leveraging telehealth’s growth, this study used a rigorously designed scientific yoga module specifically tailored for digital delivery for patients with hypothyroidism undergoing levothyroxine treatment.
Objective
This study aimed to assess the impact of a 6-month tele-yoga intervention in patients with hypothyroidism by comparing outcomes between those receiving levothyroxine combined with tele-yoga and those receiving only levothyroxine treatment.
Methods
A single-blinded, 2-arm, parallel-group randomized controlled trial was conducted for 6 months (April 1, 2022-September 30, 2022) with 134 clinically diagnosed patients with hypothyroidism recruited from the Arogyadhama Holistic Health Home registry (2013-2021). Participants were randomized to either a yoga intervention group or a waitlist control group with 67 in each group and assessed at 3 time points (before, in the middle of, and after the intervention) for primary and secondary outcomes. The 36-Item Short Form Health Survey for health-related quality of life was used as a primary measure, whereas secondary measures included thyroid profile, BMI, blood pressure, the Fatigue Assessment Scale, the Perceived Stress Scale, and the Gita Inventory of Personality. Clinical data were collected via online questionnaires, and laboratory data (thyroid profile blood pressure and anthropometric measurements) were obtained in person using standardized instruments. A generalized linear model with repeated-measure ANOVA was used to evaluate both within- and between-group effects. In addition, in the yoga intervention group, performance was assessed using a yoga performance assessment scale, and satisfaction was measured through a structured feedback survey.
Results
The intervention showed highly significant effects across all domains of the primary outcome measure (P<.001), with the most notable effects on mental health (F2, 118=425.88; η2=0.88), energy and vitality (F2, 118=371.73; η2=0.86), and role limitations—emotional (F2, 118=335.45; η2=0.85). Secondary measures also showed significant improvements (P<.001), except for thyroxine (P<.014). Average yoga performance assessment scores increased significantly from 65.08 (SD 10.97) to 88.62 (SD 11.18; P<.001), indicating that most participants could easily perform the practices. Overall, 95% (64/67) of the participants in the yoga intervention group expressed high satisfaction with the tele-yoga intervention.
Conclusions
This clinical trial is the first to demonstrate the benefits of a digitally delivered scientific yoga module combined with levothyroxine treatment for hypothyroidism. It highlights the efficacy of instructor-led tele-yoga as a scalable eHealth intervention, enhancing accessibility, long-term engagement, and sustainable health outcomes. Patients receiving tele-yoga alongside levothyroxine showed significantly greater improvements than those on levothyroxine alone, highlighting the value of integrating eHealth into thyroid care for a more comprehensive, patient-centered approach.