Improve the Rehabilitation of Cardiac Patients with Mindfulness
By John M. de Castro, Ph.D.
“Meditation practice may be clinically useful in the secondary prevention of cardiovascular disease [the prevention of further heart or stroke events for people who already have the condition].” – British Heart Foundation
Cardiovascular disease is the number one killer. A myriad of treatments has been developed including a variety of surgical procedures and medications. In addition, lifestyle changes have proved to be effective including quitting smoking, weight reduction, improved diet, physical activity, and reducing stresses. Unfortunately, for a variety of reasons, 60% of cardiovascular disease patients decline participation, making these patients at high risk for another attack.
Contemplative practices have been shown to be safe and effective alternative treatments for cardiovascular disease. Practices such as meditation, tai chi, and yoga, have been shown to be helpful for heart health and to reduce the physiological and psychological responses to stress. Additionally, they have been shown to be helpful for producing the kinds of lifestyle changes needed to prevent heart disease such as smoking cessation, and weight reduction. They have also been shown to be effective in maintaining cardiovascular health and the treatment of cardiovascular disease. Hence it is reasonable to continue studying the effects of mindfulness training on patients with cardiovascular disease.
In today’s Research News article “Randomized Trial of Mindfulness-Based Stress Reduction in Cardiac Patients Eligible for Cardiac Rehabilitation.” (See summary below or view the full text of the study at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6895078/), Niijar and colleagues performed a pilot randomized controlled trial of the effectiveness of mindfulness training for the mental and physical health of cardiovascular disease patients.
They recruited patients with cardiovascular disease who were participating in an exercise-based cardiac rehabilitation program. The patients were randomly assigned to receive either usual care or an 8-week Mindfulness-Based Stress Reduction (MBSR) program that met once a week for 2.5 hours and consisted of meditation, body scan, and yoga practices and discussion along with daily home practice. They were measured at baseline and 3 and 9 months later for depressive symptoms, anxiety, perceived stress, health-related quality of life, health history, medication usage, heart rate, heart rate variability, blood pressure, and blood triglycerides and HbA1c.
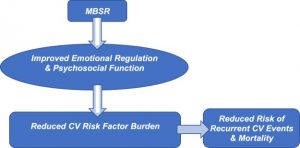
They found that in comparison to baseline and the usual care group, the group that received the Mindfulness-Based Stress Reduction (MBSR) had significantly lower levels of depression and anxiety and non-significant trends for lower levels of perceived stress and systolic blood pressure and higher levels of health related quality of life and self-rated health. They also found that the lower the levels of depression and anxiety at 3 months follow-up, the lower the cardiovascular risk factors at the 9-month follow-up, including systolic blood pressure, blood triglycerides, HbA1c, and body mass index.
This was a small pilot study that did not have sufficient statistical power to detect small group differences. In addition, all participants received exercise based cardiac rehabilitation program that would be expected to produce improvements by itself. Nevertheless, the study found that the additional participation in a mindfulness training produced significant improvements in the psychological health of the participants and also found trends toward improvements in physiological health. The results suggest that a large randomized controlled trial is justified.
The results suggest that a Mindfulness-Based Stress Reduction (MBSR) program may be an effective treatment as a supplement to exercise based cardiac rehabilitation program for the long-term improvement of the mental and physical health of these at-risk patients. This suggests that participation in MBSR in conjunction with exercise may reduce the risk of another cardiovascular event and improve the longevity and mental health of these vulnerable patients.
So, improve the rehabilitation of cardiac patients with mindfulness.
“meditation may promote heart health and reduce cardiovascular risk.” – American College of Cardiology
CMCS – Center for Mindfulness and Contemplative Studies
This and other Contemplative Studies posts are also available on Google+ https://plus.google.com/106784388191201299496/posts and on Twitter @MindfulResearch
Study Summary
Nijjar, P. S., Connett, J. E., Lindquist, R., Brown, R., Burt, M., Pergolski, A., … Everson-Rose, S. A. (2019). Randomized Trial of Mindfulness-Based Stress Reduction in Cardiac Patients Eligible for Cardiac Rehabilitation. Scientific reports, 9(1), 18415. doi:10.1038/s41598-019-54932-2
Abstract
Currently, exercise-based cardiac rehabilitation (CR) is the only recommended secondary prevention strategy for cardiac patients that attempts to tackle stress and psychosocial wellbeing, but it is under-utilized and lacks a comprehensive curriculum for this purpose; hence there is a critical gap to address psychosocial needs of cardiac patients after an event. Mindfulness-based stress reduction (MBSR) has shown benefits in the general population but its role in cardiac patients is not clear. We conducted a pilot randomized controlled trial (RCT) of MBSR in CR-eligible cardiac patients during their initial year of recovery. Patients were allocated 2:1 (intervention:control) to an 8-week MBSR group intervention or usual care. Standard measures of depression, anxiety, perceived stress, health related quality of life (HRQOL), blood pressure, biomarkers (lipids, HbA1c, CRP) and 24-hour Holter monitoring were obtained at baseline, 3- and 9-months post-randomization. Sub-group analyses were performed for participants with at least mild depression (PHQ-9 ≥ 5). 47 patients [mean age 58.6 years; 38% female; 77% white] were enrolled in 2 cohorts. 87% of MBSR patients completed the intervention; study retention was >95% at each follow-up visit. At 3 months, compared to controls, MBSR patients showed improvements in depression [p = 0.01] and anxiety [p = 0.04] with a similar trend in HRQOL [p = 0.06]. The MBSR group showed greater improvement or less worsening of most CV risk factors, with an attenuation of treatment effects at 9 months. Participants with at PHQ-9 scores ≥5 at baseline showed greater improvement in psychosocial and CV outcomes, that persisted at 9 months. MBSR is a safe and well received secondary prevention strategy. This pilot RCT provides preliminary evidence of MBSR’s potential to improve short term psychosocial well-being in cardiac patients during their first year of recovery.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6895078/