Reduce Couples Psychological Distress with Lung Cancer with Mindfulness
By John M. de Castro, Ph.D.
“Mindfulness meditation and mindfulness-based clinical interventions are low-cost and low-risk mind-body practices that have been shown to positively affect quality of life and biological outcomes in many different populations, including cancer patients and healthcare professionals.” – Susan Bauer-Wu
Receiving a diagnosis of cancer has a huge impact on most people. Feelings of depression, anxiety, and fear are very common and are normal responses to this life-changing and potentially life-ending experience. These feeling can result from changes in body image, changes to family and work roles, feelings of grief at these losses, and physical symptoms such as pain, nausea, or fatigue. People might also fear death, suffering, pain, or all the unknown things that lie ahead. So, coping with the emotions and stress of a cancer diagnosis is a challenge and there are no simple treatments for these psychological sequelae of cancer diagnosis.
But cancer diagnosis is not necessarily a death sentence. Over half of the people diagnosed with cancer are still alive 10 years later and this number is rapidly increasing. It is estimated that 15 million adults and children with a history of cancer are alive in the United States today. But, surviving cancer carries with it a number of problems. “Physical, emotional, and financial hardships often persist for years after diagnosis and treatment. Cancer survivors are also at greater risk for developing second cancers and other health conditions.” National Cancer Survivors Day.
One of the residual problems can be relationship difficulties. When one member of a couple receives a cancer diagnosis it places stress on both members and their relationship. A partner can be an asset in coping with cancer or can add to the stress exacerbating the situation. Communications and compassion become a key for couples coping with cancer. Mindfulness may be helpful. It has been shown to improve recovery from cancer and to reduce anxiety and depression in people with a wide variety of conditions. In addition, mindfulness training has been shown to strengthen relationships. So, it would make sense to study the effects of mindfulness on cancer victims, their partners and their relationship.
In today’s Research News article “Are Mindfulness and Self-Compassion Related to Psychological Distress and Communication in Couples Facing Lung Cancer? A Dyadic Approach,” see summary below or view the full text of the study at:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5355515/
Schellekens and colleagues recruited lung cancer patients and their partners. Patients were recruited at least one month after diagnosis and had either completed treatment or were currently being treated. Both partners completed measures of relationship characteristics, mindfulness, self-compassion, psychological distress, and communications about cancer.
They found that both higher levels of both mindfulness and self-compassion were related to lower levels of psychological distress in both patients and their partners and were also related to better quality of communication about the cancer, but only in patients. Neither the mindfulness or the self-compassion levels of the patients were associated with the partner’s psychological distress or visa-versa. Interestingly, the levels of self-compassion in the individual were less strongly associated with psychological distress if the partner also reported high levels of self-compassion. So, the partner’s level of compassion appears to affect the need of the individual to use their own self-compassion to mitigate psychological distress.
These results are interesting and suggest that mindfulness and self-compassion reduce psychological distress in both members of the partnership when one is diagnosed with lung cancer. They also suggest that self-compassion can also affect the partner’s processing of psychological issues, indicating a degree of influence of one partner on another. It should be noted that this study was correlational in nature and as such causation cannot be concluded. But, it does suggest that a randomized controlled trial should be conducted of the effects of mindfulness training on the psychological distress of cancer victims and their partners and how each affects the other.
So, reduce couples psychological distress with lung cancer with mindfulness.
“Studies show that patients who practice mindfulness begin to feel better despite their medical problems. Physical symptoms don’t necessarily go away, but that’s not the aim of mindfulness. Rather, the goal is to help you find a different perspective and a new way of coping with your illness.” – Eric Tidline
CMCS – Center for Mindfulness and Contemplative Studies
This and other Contemplative Studies posts are also available on Google+ https://plus.google.com/106784388191201299496/posts and on Twitter @MindfulResearch
Study Summary
Schellekens, M. P. J., Karremans, J. C., van der Drift, M. A., Molema, J., van den Hurk, D. G. M., Prins, J. B., & Speckens, A. E. M. (2017). Are Mindfulness and Self-Compassion Related to Psychological Distress and Communication in Couples Facing Lung Cancer? A Dyadic Approach. Mindfulness, 8(2), 325–336. http://doi.org/10.1007/s12671-016-0602-0
Abstract
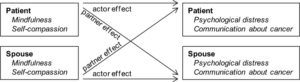
Lung cancer patients and their spouses report high rates of distress. Due to the increasing popularity of and evidence for mindfulness-based interventions in cancer, mindfulness and self-compassion have been identified as potentially helpful skills when coping with cancer. This dyadic study examined how mindfulness and self-compassion are related to psychological distress and communication about cancer in couples facing lung cancer. Using the actor-partner interdependence model, self-reported mindfulness, self-compassion, psychological distress and communication about cancer were analyzed in a cross-sectional sample of 88 couples facing lung cancer. Regarding psychological distress, no difference was found between patients and spouses. In both partners, own levels of mindfulness (B = −0.19, p = .002) and self-compassion (B = −0.45, p < .001) were negatively related to own distress levels. At a dyadic level, own self-compassion was less strongly associated with distress if the partner reported high self-compassion (B = 0.03, p = .049). Regarding communication about cancer, patients reported to communicate more openly with their partner than with spouses. However, after controlling for gender, this difference was no longer significant. In both partners, own self-compassion (B = 0.03, p = .010) was significantly associated with own communication while mindfulness was not. A trend showed that mindfulness of the partner was related to more open communication in the individual (B = 0.01, p = .080). These findings give a first indication that mindfulness and self-compassion skills may go beyond the individual and could impact couple functioning. Future research should examine whether couples facing (lung) cancer may benefit from programs in which mindfulness and self-compassion are cultivated.
One thought on “Reduce Couples Psychological Distress with Lung Cancer with Mindfulness”