By John M. de Castro, Ph.D.
“Stress is a primary instigator of symptoms associated with Parkinson’s Disease. A practical and powerful way to reduce stress is to become more mindful which, simply put, means we are present in the moment rather than agonizing over the past or anticipating the future.” – Robert Rodgers
Parkinson’s Disease (PD) has received public attention because of its occurrence in a number of celebrities such as Mohammed Ali, Michael J Fox, and Linda Ronstadt. PD is an incurable disease of the central nervous system that attacks the dopamine neurotransmitter system in the brain. There are around seven million people worldwide and one million people in the U.S. living with PD and about 60,000 people are diagnosed with PD every year. PD is associated with aging as the vast majority of patients are diagnosed after age 50. In fact, it has been speculated that everyone would eventually develop PD if they lived long enough.
PD is an incurable progressive degenerative disease. The condition is caused by the death of nerve cells in the brain that produce the neurotransmitter dopamine. Its physical symptoms include resting tremor, slow movements, muscle rigidity, problems with posture and balance, loss of automatic movements, and slurring of speech. PD itself is not fatal but is often associated with related complications can reduce life expectancy, such as falls, choking, and cardiovascular problems. There are also psychological effects, especially anxiety and depression. All of these symptoms result in a marked reduction in the quality of life.
Mindfulness training has been found to improve the psychological symptoms and the quality of life with PD patients. But, because PD is caused exclusively by a physiological degeneration it would be surprising if mindfulness practice can help improve the physical symptoms. But, in today’s Research News article “Mindfulness for Motor and Nonmotor Dysfunctions in Parkinson’s Disease.” See:
or below or view the full text of the study at:
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4842053/
Dissanayaka and colleagues investigated if mindfulness training could improve not only the psychological symptoms and the quality of life but also the physical symptoms of Parkinson’s Disease (PD). They treated PD patients for 8 weeks with a version of the Mindfulness Based Stress Reduction (MBSR) program that was adapted for PD. Measurements of physical and psychological symptoms were obtained before and after treatment and 6 months later.
They found that after mindfulness training there was a significant improvement in anxiety, depression and psychological distress. Cognitive ability also improved including improvements in memory and verbal fluency. These results are compatible with these shown in previous research on mindfulness training for PD patients. These are important effects as they reduce quality of life and can lead to suicidal thoughts. It can be speculated that these effects on psychological well-being were due to the known effects of mindfulness training on emotion regulation. These involve the full experience and recognition of the emotions, but with adaptive responses to them. So, the patients don’t deny how they feel but do not react to them negatively, instead cope with the feelings and act positively.
Of the physical symptoms, they observed improvement in postural instability gait dysfunction but not tremor. This is surprising as these motor symptoms are due to direct deterioration of the neural systems underlying movement. It is possible that the yoga component of MBSR may have improved strength, balance, and flexibility and thereby improved the posture and gait of the PD patients even though the underlying brain degeneration was not affected.
The psychological and motor improvements that were present immediately after mindfulness training were no longer present six months later. But, it should be noted that PD is a progressive disorder, with symptoms getting worse over time, which could have obscured the improvements detected after treatment. The study lacked an untreated control condition, so it is impossible to determine whether the continued deterioration produced the lack of effects at the 6-month follow-up. It should also be noted, however, that the lack of a control condition limits the conclusion that the mindfulness training was responsible for the improvements and not another confounding variable such as a placebo effect or experimenter bias.
Regardless, it is clear that both the psychological and motor symptoms of Parkinson’s Disease can be improve with mindfulness training.
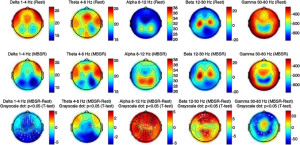
“You would expect mindfulness-based interventions to alleviate the psychological symptoms of Parkinson’s – mindfulness has proved its worth at reducing both anxiety and depression – but a recent study suggests mindfulness training could also address some of the physical changes in the brain. An eight-week course of mindfulness training seemed to increase the density of grey matter in two areas of the brain associated with the disease.” – Plastic Brain
CMCS – Center for Mindfulness and Contemplative Studies
This and other Contemplative Studies posts are available on Google+ https://plus.google.com/106784388191201299496/posts
Study Summary
Dissanayaka, N. N. W., Idu Jion, F., Pachana, N. A., O’Sullivan, J. D., Marsh, R., Byrne, G. J., & Harnett, P. (2016). Mindfulness for Motor and Nonmotor Dysfunctions in Parkinson’s Disease. Parkinson’s Disease, 2016, 7109052. http://doi.org/10.1155/2016/7109052
Abstract
Background. Motor and nonmotor symptoms negatively influence Parkinson’s disease (PD) patients’ quality of life. Mindfulness interventions have been a recent focus in PD. The present study explores effectiveness of a manualized group mindfulness intervention tailored for PD in improving both motor and neuropsychiatric deficits in PD. Methods. Fourteen PD patients completed an 8-week mindfulness intervention that included 6 sessions. The Five Facet Mindfulness Questionnaire (FFMQ), Geriatric Anxiety Inventory, Hamilton Depression Rating Scale, PD Cognitive Rating Scale, Unified PD Rating Scale, PD Quality of Life Questionnaire, and Outcome Questionnaire (OQ-45) were administered before and after the intervention. Participants also completed the FFMQ-15 at each session. Gains at postassessment and at 6-month follow-up were compared to baseline using paired t-tests and Wilcoxon nonparametric tests. Results. A significant increase in FFMQ-Observe subscale, a reduction in anxiety, depression, and OQ-45 symptom distress, an increase in PDCRS-Subcortical scores, and an improvement in postural instability, gait, and rigidity motor symptoms were observed at postassessment. Gains for the PDCRS were sustained at follow-up. Conclusion. The mindfulness intervention tailored for PD is associated with reduced anxiety and depression and improved cognitive and motor functioning. A randomised controlled trial using a large sample of PD patients is warranted.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4842053/